Knee arthroscopy is one of the most frequently used procedures for the diagnosis and treatment of knee injuries. Arthroscopy is term used when I look inside your knee joint with a small telescope and video camera. The image is projected onto a television monitor using a fibreoptic light source and a digital camera. This modern technique allows me to fully inspect all of the interior structures of your knee joint without needing open surgery. Despite the fact that the incisions are quite small, a large amount of surgery can be performed within the knee. Since only small incisions are made, you usually have an arthroscopy as an outpatient. This means, you can go home the same day you have your surgery.
Click here to watch an animation of a knee arthroscopy
What are the benefits of knee arthroscopy?
Knee arthroscopy is an effective tool to treat knee problems such as meniscus tears and cartilage wear. An arthroscopy can usually provide relief from knee pain and improve mobility. For most people this means maintaining a normal and active lifestyle with greater comfort.
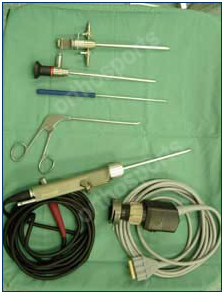
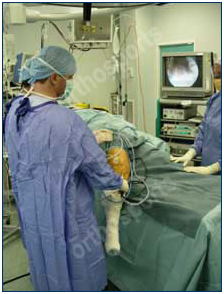
Instruments used and typical setup in the operating theatre.
What are the indications for knee arthroscopy?
Knee arthroscopy can be used to trim or repair a torn meniscus, remove loose bodies or floating fragments, take samples of the joint lining (synovial biopsy), perform an ACL reconstruction, washout blood after a knee injury, debride (perform a ‘spring cleaning’) arthritis, diagnose and treat patella or kneecap instability or arthritis and harvest cells for cartilage grafting.
Meniscal Injury…
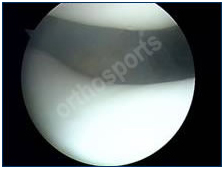
Meniscal injury is the most common reason for you to need an arthroscopy and twisting your knee joint is the most common cause of a torn meniscus. The meniscus (sometimes known as ‘the cartilage of the knee’) acts as a shock absorber in the knee. The torn part of the meniscus can be a source of pain and further damage to the joint (see Meniscal Tears). A torn meniscus can cause catching of the knee, locking of the knee, giving way or buckling (instability) of the knee, pain or swelling. The size and location of the tear of the meniscus determine both treatment and recovery. The meniscus serves a useful function and I always strive to repair it to preserve the long term function of your knee.
If your meniscus is torn and is not repairable then a segment of the meniscus is removed. The larger the fragment of meniscus removed the greater the chance of developing arthritis of the knee in the long term. Sometimes in younger patients the meniscus can be repaired (see meniscal repair). While this is usually done through the keyhole cuts there are times when a larger cut is required to get a solid repair. The recovery time is longer (up to 6 months for return to sport) and a splint and crutches may be required.
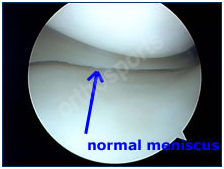
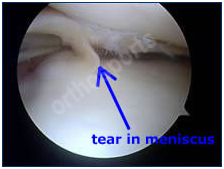
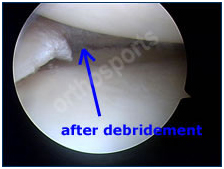
Meniscal tear as seen during arthroscopy before and after trimming.
To view an operative video of Arthroscopic Meniscal Debridement, click here.
Articular Cartilage…
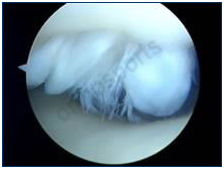
The parts of your knee bones that touch each other are covered with a smooth lining material called articular cartilage. The joint lining cartilage protects the bones from each other as the joint moves and the bones rub. This allows your bones to move freely against each other without friction or pain. If the smooth surfaces become rough or irregular they can cause pain and swelling in your knee – this is the earliest form of arthritis. Arthroscopy can help with this by removing loose flaps of cartilage or smoothing over rough areas which are catching or breaking dow.
Unfortunately this is less reliable than treating a meniscal tear. It is not possible for an arthroscopy to cure arthritis but it can provide some relief for months or even years. Typically recovery is less than complete and occasionally the results are disappointing but most patients tell me that they are glad they had the procedure done.
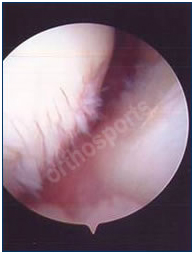
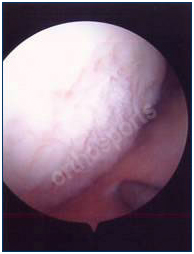
Chondral damage before and after debridement.
To view an operative video of Arthroscopic Chondral Shaving,click here.
Loose Bodies…
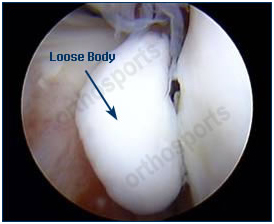
If a piece breaks free inside your knee it is called a loose body. Typically loose bodies are pieces of joint lining cartilage, meniscus or bone and can occur from a variety of causes. Some people describe a ‘mouse’ in their knee and are able to feel the loose piece moving around. If the loose piece jams in the joint the knee can ‘lock up’. These are removed during knee arthroscopy which fixes the problem.
Diagnosis…
There are times that your diagnosis may not be clear despite having had very sophisticated tests such as an MRI scan or CT scan. I will then carefully examine your knee under anaesthetic (while you are asleep) and perform a knee arthroscopy. This may allow me to diagnose a ligament tear, injury to your bone or articular cartilage (lining of the joint) or perform a biopsy of the synovium. Arthroscopy is useful to assess the inside of the knee to determine the suitability for other surgical procedures such as a high tibial osteotomy, ACL reconstruction, or MPFL Reconstruction (patella ligament reconstruction).
Patella (Knee Cap) Pain…
Patella pain (knee cap pain, anterior knee pain) almost always responds well to physiotherapy. The results of arthroscopic surgery for anterior knee pain are unpredictable but sometimes removing loose fragments from the knee or smoothing the rough patella chondral cartilage can help.
If your patella does not sit properly in it’s groove on the thigh bone (trochlear) you might have a tight lateral retinaculum. Releasing this tight structure can relieve the pressure on your kneecap. The operation is called an arthroscopic lateral release and takes longer to recover from than a standard knee arthroscopy.
Arthritis…
Arthritis can occasionally be helped by arthroscopy, especially if there are recent mechanical symptoms (i.e. locking, clicking). This is what we regard as a ‘grease and oil’ change for a knee that will eventually require a total knee replacement.
Anterior Cruciate Ligament Reconstruction…
See ACL reconstruction for further information.
Cartilage Biopsy…
A knee arthroscopy can be used to diagnose your injury and to harvest some of the normal cartilage cells from your knee. A piece of normal cartilage about the size of a tic tac is taken from an area in which it is not needed. This is then sent to a laboratory where it is cultured (a small number of cartilage cells are grown and multiplied into a large number of cells). These cells are grown in a membrane which is stored for later use.
Results
The results from arthroscopic surgery depend on the arthroscopic findings and the underlying condition. In cases of a torn meniscus with no other damage to the joint, the results are usually excellent (There may be a long term tendency towards arthritis since one of the shock absorbers of the joint has been damaged).
Patients who are found to have damage to the articular cartilage (which lines the joint), are likely to continue to experience symptoms. This is due to the underlying nature of the condition and may be intermittent. Patients who have osteoarthritis are unlikely to gain full relief of symptoms following arthroscopic surgery. Arthroscopic surgery in the presence of osteoarthritis can help if the meniscus is torn or there is loose cartilage in the joint but does not affect the underlying condition, which is likely to gradually progress. Occasionally arthroscopic surgery in the presence of osteoarthritis can make symptoms worse for a period of months. Results in these cases are occasionally disappointing with worsening of symptoms but can provide excellent relief for some patients.
Preparing For Your Operation
Exercise
It is useful to do some quadriceps exercises prior to your operation. These exercises are designed to maintain muscle strength of the quadriceps group (which are your front thigh muscles). It is very important to also continue these exercises after your operation.
Exercise up to the point of mild discomfort is reasonable and is unlikely to cause any damage inside the knee.
Medical History and Medications
Please complete a health questionnaire at the time of your consultation and prior to your operation. I require information about your past and present illnesses, previous operations, current medications and any known allergies. A blood test may be needed for some patients.
It is important that you inform me of any change in your medications or health status.
Please take a list of your current medications and known allergies to the hospital on the day of admission and provide this to the anaesthetist, who will see you before your operation.
Anti-inflammatory medication such as Aspirin, Orudis, Feldene, Voltaren and Naprosyn should be stopped 10 days prior to surgery as they can cause bleeding. Celebrex and Mobic may be continued until the day before the procedure and if you have any doubts check with me or my staff.
You are advised to stop smoking for as long as possible prior to surgery.
Cease any naturopathic or herbal medications 10 days before surgery as these can also cause bleeding.
Continue with all other medications unless otherwise specified.
Notify me if you have any abrasions or pimples around the knee as this may increase your infection rate and we may need to delay the surgery until the skin is healed.
Please bring any X-rays, MRI scans or other investigations of your knee with you to the hospital. Arrange for a responsible adult to drive you home after surgery and stay with you the first night after surgery. It is best to wear loose-fitting shorts or non-constricting pants (warm-up style) that will fit over your dressing after surgery.
The operation is usually performed under a general anaesthetic but the final decision rests with the anaesthetist.
The Operation
You will be admitted to hospital on the day of your operation.
You will need to phone the hospital on the working day prior to you operation to be advised of the admission time to hospital. You will also be given fasting instructions (you will be told how long before your operation you not eat or drink).
The anaesthetist will see you before your operation. You will need to discuss with the anaesthetist your medical history, current medications and any previous anaesthetic problems. Please feel free to discuss with the anaesthetist the type of anaesthetic that will be used (usually a general anaesthetic) and its possible side effects and complications.
The operation is usually performed under general anaesthesia (i.e. you are asleep). At the end of the procedure the knee is injected with long acting local anaesthetic to keep pain to a minimum.
At the end of your operation you will be taken to the recovery room. You usually stay here for an hour or so, depending on your type of surgery. You will be in recovery until the effects of anaesthetic have worn off and you are reasonably free of pain.
Your vital signs are closely monitored. You may be given fluids and medicines for pain or nausea from the anaesthetic. You will have an ice pack on your knee to help reduce pain and swelling. Your circulation and nerve function will be checked regularly.
Discharge – Going Home
I will see you to explain the operation to you before you leave the hospital.
You may have a big bandage, brace, or ice pack on your knee. It may take several hours for the knee to feel normal again. Be careful not to bump or injure your knee and spend most of the day with your leg elevated, doing as little walking as possible. You will be seen by a physiotherapist either before or after you operation to teach you how to walk after your operation. You will be shown some exercises to do. If crutches are required they will be supplied by the hospital physiotherapist.
Recovery At Home
Knowing how to care for your knee once you get home will make a big difference in your recovery and results. How fast your knee heals depends on your age, your job, your fitness level before surgery, how active you are or want to be, and how much time you’re willing to spend on getting your knee back to normal. Everyone’s recovery time is based on their overall health and the extent of their knee surgery.
An ice pack will be applied to the knee, which will also help prevent swelling and pain. Please leave the bandage in place for at least 24 hours while applying ice to the knee. You will be given instructions for wound care when you leave the hospital.
I suggest you use the pain killers on the night of the operation even if you do not have much pan. The local anaesthetic tends to wear off during the night and the knee remains comfortable if you already have the pain killers on board.
You may exercise at home up to the point of mild discomfort. This is unlikely to cause any damage to your knee. Avoid deep squats, kneeling and spending too much time on your feet in the first few days after surgery. It is important to keep the leg elevated as much as possible for 3 or 4 days.
It is normal for some blood to collect under the dressings. It is also normal for the knee to develop some bruising after surgery.
You will be provided with pain killers to take home with you. These are designed to minimise but not completely eliminate knee pain. You should feel mild discomfort only. Do not attempt to drive or attend work or school while taking pain medication.
If you take regular anti-inflammatory medications, you may resume these after surgery.
Driving
It is not permitted to drive a motor vehicle for 24 hours after having a general anaesthetic. You will therefore need to arrange other transport home from the hospital. It is best to go home with a relative or a friend. You can resume driving only when your knee is comfortable and you have no restrictions in operating your vehicle.
It is recommended that you do not travel long distances by car or plane for at least two and preferably six weeks following surgery as prolonged travel can increase the risk of forming blood clots in the leg.
I will need to see you in my office about 10 days after surgery.
How long is the recovery period after knee arthroscopy?
Return To Work
You may return to work as your knee function improves well enough for you to do your particular job. This does not mean that all discomfort must have resolved, as there will be some tenderness around the wounds. It is normal for there to be some discomfort in the knee for several weeks after arthroscopic surgery. I will provide you with an extension of your medical certificate at your first post-operative visit if required.
Early Recovery
Recovery from this operation involves reducing the swelling, strengthening the muscles and reducing pain.
Reduce Pain
Excessive pain in the knee following arthroscopic surgery is usually due to overactivity or spending too much time on your feet before the thigh muscles have been adequately strengthened. Excessive swelling can also cause pain in the knee.
It is normal for the knee to be sore and swollen following arthroscopy. Activity should be increased gradually. You should avoid prolonged walking or standing for the first few days. You should avoid squatting or kneeling or attempting to bend your knee beyond 90 degrees if the knee is painful or swollen.
Reduce Swelling
Keep the leg elevated as much as possible after the operation. Try to elevate your knee higher than your heart level on two or three pillows with your back flat on the bed. Apply ice to the knee continuously when the initial post operative bandage is in place and then for about 30 minutes at a time once this has been removed. Initially the ice packs should be placed on the bandages and then when the dressing has been reduced ensure that you place a cloth between your skin and the ice pack to prevent an ice burn. Anti-inflammatory medications can also be helpful in reducing swelling.
Quadriceps Strengthening Exercises
Strengthening your quadriceps is important in restoring function to the knee.
The physiotherapist at the hospital will have shown you how to do these exercises. You should continue them on a regular basis for several weeks after the operation.
Following surgery, you will wake up in recovery with your knee bandaged. Most patients will go home on the day of surgery, but some may require an overnight stay. You will require pain killers and may have crutches to go home. You should make arrangements to get home, as you will not be able to drive.
You will usually be seen before you go home to explain the results of the operation. This will be further discussed at your follow up visit.
Complications
Any surgical procedure has a risk of complications. These are rare with an arthroscopy, however they can occur. Every precaution is taken to minimise the risk. Complications can be related to the anaesthetic, general in nature it can happen with any surgery or be specific to knee arthroscopy.
Arthroscopy of the knee is a safe and effective procedure. Remember that every knee is unique, and recovery time and the results of the procedure reflect this. Complications are rare but can occur. If you have further questions regarding your surgery, please ask before your operation.
Phase 1
Exercises during this early phase help patients regain balance and coordination and should be started immediately following discharge from the hospital.
The isometric quadriceps exercise (also known as “quad sets”) may be started in the sitting or lying position. During the exercise, press your knee down against a table or floor, holding the position for 6 seconds. The exercise can be repeated 10 to 15 times for each set. Two to three sets should be completed in each exercise period.
The straight leg raising exercise is done sitting or lying. The ankle of the leg to be exercised should be bent at a 90-degree angle, and the knee is straightened as much as possible. Then, the entire leg and thigh are lifted off the floor to a height of approximately 1 to 1-1/2 feet and held in the air for 6 seconds. The exercise should be repeated 10 to 15 times for each set; two to three sets should be completed in each exercise period. Patients may add weights for this exercise, beginning with 2 lb weights and adding increments of 1-2 lbs.
Phase 2
These exercises help patients regain full knee motion and strength once they discontinue using crutches.
The range of motion exercise is done by sitting on the table and letting the leg hang over the edge. Patients may use their good leg to help straighten (extension) and bend (flex) the knee.
Patients can begin doing bicycle exercises on a stationary bicycle as soon as the knee has a fairly good range of motion.
Short arc quadriceps extensions are used for the development of the quadriceps muscle. To perform this exercise, patients should be lying down with the unaffected knee bent placing a flat foot on a resting surface. The affected knee is supported off the table by a firm, padded object. The knee is then extended fully to zero degrees from its bent position of approximately 30 to 40 degrees. The leg is then held straight for 6 seconds and then gently lowered.
Initially, no ankle weights are used for this exercise, but as patients gain strength, they may choose to add weight to the ankle. Patients can start with 2 lbs and add increments of 1-2 lbs.
The knee flexion exercise is done while lying face down. The foot is rested on a rolled towel to prevent the toes from striking the table. The foot is slowly raised and lowered to the table. Initially, no weights are used, but as the patient’s knee gains strength weights may be added.
Phase 3
When patients have reached Phase 3 of the physical therapy program, they will be ready to return to normal physical activity. The length of time leading up to this phase depends on the individual patient and their recovery progress following surgery.
During knee arthroscopy, the damaged part of the meniscus can either be repaired or removed to prevent permanent damage to the knee joint. If the tear is near the edge, the meniscus may be trimmed to smooth the rim. In most cases, it will be repaired with stitches which can make rehab longer, but your knee will better keep its shock absorbing ability. You’ll need crutches, a brace to immobilize your knee, and limited weight bearing. A full recovery is likely for a mild injury. If the meniscus was removed, you may have more problems in the future.